K•S Blog
Call Us Today
(763) 746-7800
Get a Free Consultation
Contact
Keeping a Loved One in a Nursing Home Safe From Coronavirus
By wpengine / March 6, 2020
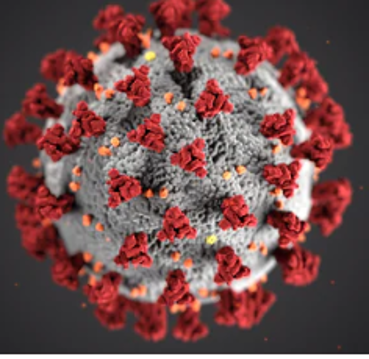
What is the Coronavirus?
The Coronavirus, now named COVID-19, is a new virus not previously known to infect humans. The coronavirus family is a big family: some coronaviruses are known to infect humans, and some of those can cause minor symptoms like a common cold.
Other coronaviruses only infect animals, but not humans.
Rarely, an animal-only coronavirus changes and starts to infect humans. This has happened before; examples are SARS (Severe Acute Respiratory Syndrome) and MERS (Middle East Respiratory Syndrome).
COVID-19 appears to be similar to the SARS coronavirus.
How Does COVID-19 Spread?
Although COVID-19 originally spread from animals to humans, now it is spreading human-to-human. The main way it is spread is through respiratory droplets: those tiny liquid droplets that shoot out and scatter when you sneeze or cough.
COVID-19 can also be contracted by touching a surface that an infected person coughed or sneezed on, but this isn’t thought to be the main way it is transmitted.
A person with COVID-19 who has a fever and is coughing is infectious and can spread the infection to other people. It is also possible that infected persons can spread COVID-19 infection before they develop fever and cough.
With other coronaviruses, a person who is going to get sick usually does so within 14 days of being exposed, so it is a good guess that this will be true for COVID-19.
Does the Government Protect Nursing Home Residents from Infections Like COVID-19?
Most of the first deaths in the United States from COVID-19 were of residents of a long-term care facility in Washington state.
The federal government has issued new guidelines in an attempt to keep nursing home residents safe from COVID-19.
The new federal guidelines, issued in a paper called a “guidance” (CMS Guidance Ref: QSO-20-14-NH), direct nursing homes to do the following:
- Screen nursing home visitors for travel to countries where there are lots of COVID-19 infections, for contact with infected people, or for symptoms compatible with COVID-19 infection; do not allow visitors who are positive for any of those screening questions to enter the nursing home.
- Screen nursing home staff in the same way, and do not allow them to come to work if they are positive for any screening questions.
- Notify the local health department about suspected COVID-19 infections.
- Accept COVID-19-infected residents only if Centers for Disease Control and Prevention guidelines are followed.
- It is okay to admit non-infected residents who come from facilities where COVID-19 was present.
- Increase availability of hand-sanitizer, face masks, and tissues.
- Post signs to remind staff of infection prevention measures.
- Clean and limit sharing of medical equipment and workplaces.
A second new federal “guidance” (CMS Guidance Ref: QSO-20-12-All) informs nursing homes that the federal government will be sending inspectors to nursing homes with serious deficiencies that place residents’ health in jeopardy, or which have residents with respiratory infections that potentially could be COVID-19.
Did the Government Do Anything to Protect Nursing Home Residents from Infection Before COVID-19?
The federal government has long-standing regulations directing nursing homes to have infection prevention and control programs to protect residents from infectious diseases: 42 CFR § 483.80. The Centers for Medicare and Medicaid Services publishes details of their requirements for the infection prevention and control program for nursing homes, as a “Guidance to Surveyors” (listed under F-TAG# F880). Under these regulations, nursing homes are required to have standardized written policies, to include things like:
- preventing sick staff from infecting residents;
- hand-washing rules;
- hygienic cleaning and handling of linens;
- rules about when a sick resident should be isolated from other residents;
- ways to prevent one resident from spreading infection to another; and
- ways to prevent visitors from infecting residents.
How Do I Know if the Nursing Home is Following the Federal Rules to Protect Residents from COVID-19?
These are things you can look for to see if the nursing home where your loved one lives is following the federal government’s guidelines:
- Staff should be at the nursing home entrance asking each visitor about travel, contact with sick persons, and symptoms of infection.
- The nursing home should have strict rules to prevent staff who are sick from coming into the nursing home.
- Hand-sanitizer stations should be placed throughout the nursing home.
- Signs should be posted, reminding staff to wash their hands.
- New residents should be carefully screened for symptoms of COVID-19.
- Surfaces and medical equipment should be frequently disinfected.
- Staff should wash their hands frequently, and always before and after touching a resident.
- Residents with infectious symptoms should be kept away from other residents.
Why Are Nursing Home Residents Especially at Risk for COVID-19 Infection?
Nursing home residents are often frail, and this makes them especially susceptible to infections such as COVID-19. Additionally, they live in a residence that often requires them to be in close contact with the other residents, as well as staff. They do not have the option of staying 6 feet away from others who might be sick.
Nursing home residents are often dependent upon others for much of their care. They may require staff to wash their hands for them.
Nursing home residents are counting on staff to follow handwashing rules and not spread germs from resident to resident. Unfortunately, nursing home staff do not always wash their hands between caring for different residents. For example, in Minnesota, the Centers for Medicare and Medicaid Services cited North Ridge Health and Rehab in a public document called a “Survey,” in years 2016, 2017, and 2018, for deficiencies related to staff not following “proper hand hygiene”.
Nursing home residents do not have control over their environment. They count on staff to disinfect surfaces and to keep them safe from infected visitors.
Often, nursing home residents are not able to make decisions for themselves and may be unaware that they are touching their face, or that they have not had their hands washed before eating or after toileting.
On top of the special vulnerabilities that nursing home residents have, nursing homes may be understaffed, and their staff might not have been properly trained, further increasing the risk to the residents. In the federal Survey of North Ridge Health and Rehab mentioned above, one of the staff members, who had failed to do proper handwashing, told the investigator in 2018: “I am supposed to wash them. I am so behind and this happens all the time and I always have to help everyone.”
What Can I Do to Keep My Loved One in a Nursing Home Safe from Getting COVID-19?
You can help keep your loved one safe. If you have a loved one in a nursing home, consider taking these steps:
On your computer, go to Medicare.gov/nursinghomecompare/ and enter the name of the nursing home where your loved one resides. There, you can learn if that nursing home is better or worse than the national average for health deficiencies.
Visit the nursing home. Look for these things:
- When you arrive, does a staff member ask you about your travel or symptoms of infection before they let you enter?
- Do you see frequent hand sanitizer stations available to visitors?
- Do you see residents placed close together when one is coughing, sneezing, or displaying other infectious symptoms?
When you are at the nursing home, observe the staff. These are things to look for:
- Are the staff frequently washing their hands? Do they wash their hands between touching residents?
- Do you see staff washing their hands before touching your loved one? Do they clean their equipment, like stethoscopes, before touching them to your loved one?
- Do you see staff disinfecting a surface after a contaminated article (such as soiled linens) are placed upon it?
- Do staff take the time to clean your loved one’s hands before your loved one eats? After your loved one is toileted? After your loved one coughs or sneezes?
- Do you observe any staff who appear ill?
Ask the staff:
- “Did you wash your hands?” before they touch your loved one.
- Ask to see their written policy on infection control; ask if there have been updates to deal with the coronavirus. (The rules regarding sharing of these policies with residents/families are state-specific: in Minnesota, a nursing home must make their policies available for residents to see, as part of the Health Care Bill of Rights, Minn. Stat. § 144.651, subd. 4.)
What Do I Do if My Loved One Has Been Harmed by the Nursing Home?
The Kosieradzki Smith Law Firm has experience representing residents of nursing homes, and families of nursing home residents, when a loved one has been harmed by a nursing home or assisted living facility.
If your loved one in a nursing home has been the victim of abuse or neglect, including if your loved one has developed an infection due to the fault of the nursing home or assisted living facility, the Kosieradzki Smith Law Firm is here to help you take action to protect your loved one and to bring a claim against the responsible parties.
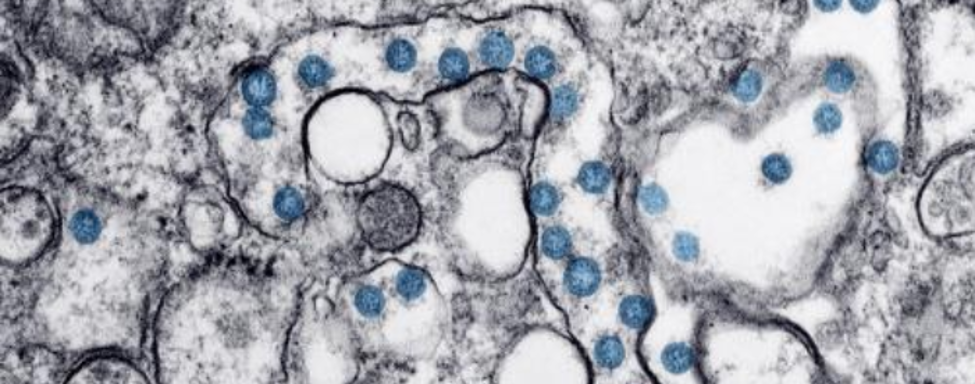
Centers for Disease Control and Prevention.